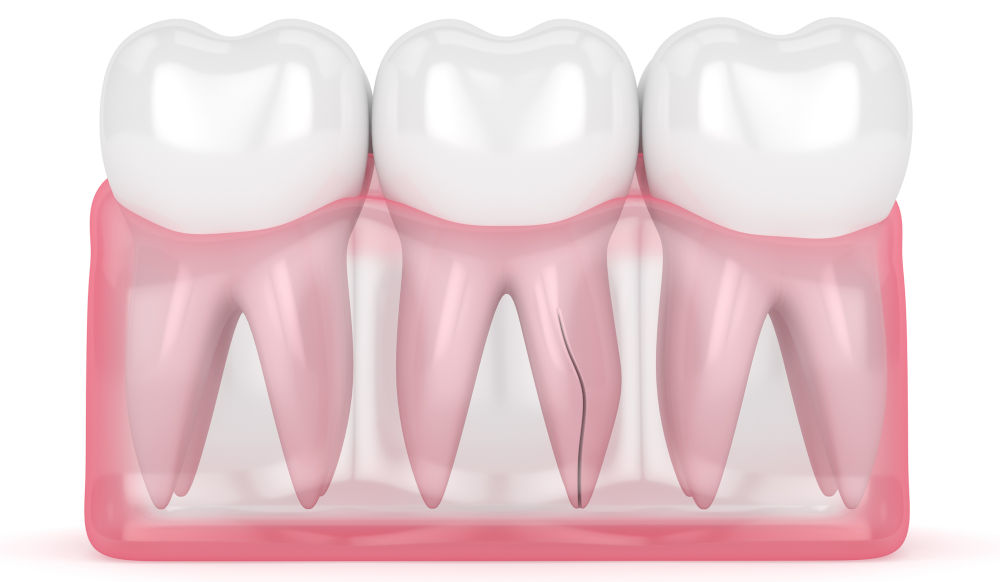
Cracked teeth rarely announce themselves clearly. Instead, they reveal subtle, inconsistent symptoms that are easy to dismiss until the damage progresses. Patients often report pain when chewing, sensitivity to temperature, or discomfort that comes and goes without a clear cause. Early detection is critical, as untreated cracks can deepen, leading to infection or tooth loss. Clinical literature consistently shows that symptom variability is a major challenge in diagnosing cracked tooth syndrome.
Key Takeaways
- Pain when biting or releasing pressure is one of the most common indicators
- Sensitivity to hot, cold, or sweet foods may signal structural compromise
- Symptoms can be intermittent, making diagnosis more complex
- Hairline cracks may produce minimal or delayed symptoms
- Early professional evaluation significantly improves treatment outcomes
What are the most common cracked tooth symptoms you should watch for?
Cracked teeth rarely follow a predictable pattern. One patient may experience sharp, immediate pain when chewing, while another may notice only mild sensitivity over several weeks. This inconsistency is precisely what makes cracked tooth syndrome difficult to identify without a thorough dental evaluation.
Pain When Chewing or Biting
One of the most frequently reported symptoms is discomfort when biting down. Interestingly, the pain often occurs not during the bite itself but when the pressure is released. This happens because the crack allows parts of the tooth to shift slightly under pressure, irritating the inner pulp.
Patients often describe this sensation as:
- A sharp, localized pain
- A sudden “zing” when chewing certain foods
- Discomfort that disappears quickly after the bite
According to research published in the Journal of Endodontics, pain on release is a hallmark diagnostic feature of cracked teeth, distinguishing it from other dental conditions.
Sensitivity to Temperature and Sweet Foods
Temperature sensitivity is another key indicator. Cold beverages, hot drinks, or sugary foods may trigger discomfort that lingers longer than usual. This occurs because cracks expose the dentin layer, which contains microscopic tubules leading to the tooth’s nerve.
But here’s where it gets tricky: this sensitivity may not be constant. Some days, the tooth feels completely normal. On other days, even mild temperature changes cause noticeable discomfort.
Intermittent and Unpredictable Discomfort
One of the most frustrating aspects for patients is the inconsistency of symptoms. The pain may appear for a few days, disappear entirely, and then return without warning.
This variability is well-documented in clinical studies, which highlight that cracked tooth syndrome often presents with:
- Irregular pain patterns
- Difficulty identifying the exact tooth
- Symptoms that worsen over time if untreated
Early vs Advanced Symptoms
Early-stage cracks are often limited to the enamel and may produce minimal symptoms. Patients might only notice occasional sensitivity or slight discomfort when chewing harder foods.
As the crack progresses deeper into the dentin or pulp, symptoms become more pronounced:
- Increased pain intensity
- Longer-lasting sensitivity
- Possible swelling or infection if the pulp is affected
In advanced cases, the tooth may require root canal therapy or extraction if structural integrity is compromised.
What does a cracked tooth feel like in daily life?
Living with a cracked tooth is less about constant pain and more about unpredictability. Patients often adapt their habits without even realizing it, chewing on one side, avoiding certain foods, or hesitating before taking a bite.
Sharp, Sudden Pain During Everyday Activities
Imagine biting into something as simple as bread or a granola bar and feeling a quick, sharp pain. That’s one of the most common real-life experiences.
The sensation is often described as:
- Brief but intense
- Difficult to reproduce on demand
- Triggered by specific angles or pressures
This inconsistency can make patients question whether the issue is serious, delaying diagnosis.
Pressure Sensitivity and Functional Limitations
Over time, many patients begin to notice discomfort when applying pressure to the affected tooth. This can lead to subtle behavioural changes:
- Avoiding chewing on one side of the mouth
- Preferring softer foods
- Being cautious with crunchy or hard textures
These adaptations often develop gradually, making them easy to overlook.
Temperature Triggers in Daily Routines
Hot coffee in the morning or cold water after exercise, these everyday moments can become triggers. The tooth may react with sudden sensitivity disproportionate to the stimulus.
Research from the American Association of Endodontists indicates that temperature sensitivity is frequently associated with cracks that extend into the dentin, even when no visible damage is present.
Variability of Pain: Why It Comes and Goes
A defining characteristic of cracked teeth is variability. Pain may depend on:
- The direction of the bite
- The type of food
- The depth and orientation of the crack
Dr. Blair Farbstein notes that, “Cracked teeth are particularly challenging because symptoms don’t always match the severity of the damage. A minor crack can cause significant discomfort, while a deeper fracture may go unnoticed until complications arise.”
This mismatch often leads patients to delay seeking care, assuming the issue will resolve on its own.
Can a hairline crack in a tooth cause noticeable symptoms?
Hairline cracks, also known as craze lines or microcracks, are among the most difficult dental conditions to detect. They may not appear on standard X-rays and often require magnification or specialized diagnostic tools.
Subtle and Often Overlooked Signs
Unlike larger fractures, hairline cracks may not cause immediate pain. Instead, patients might notice:
- Mild sensitivity to cold
- Occasional discomfort when chewing
- A vague awareness that something feels “off.”
These symptoms are easy to dismiss, especially when they are infrequent or mild.
Why Microcracks Are Hard to Detect
Microcracks can run in unpredictable directions and may only open under specific pressure conditions. This means that during a routine exam, the tooth might appear completely normal.
Dentists often rely on a combination of techniques to identify them:
- Bite tests using specialized tools
- Transillumination (shining light through the tooth)
- Magnification with dental microscopes
Clinical literature highlights that early detection significantly reduces the risk of crack propagation.
Delayed Pain and Progressive Damage
One of the most concerning aspects of hairline cracks is the delayed onset of symptoms. A tooth may remain asymptomatic for months before suddenly becoming painful.
Clinical Insight: How Dentists Approach Microcracks
From a clinical perspective, diagnosis often depends on patient-reported symptoms combined with targeted testing. Dentists evaluate patterns rather than relying on a single indicator.
In practice, this means:
- Tracking when pain occurs
- Identifying specific triggers
- Comparing responses across multiple teeth
Early intervention, such as placing a crown, can stabilize the tooth and prevent further damage.
Comparison of Cracked Tooth Symptoms by Severity
| Symptom Type | Early Stage Crack | Moderate Crack | Advanced Crack |
|---|---|---|---|
| Pain when chewing | Occasional | Frequent | Severe and persistent |
| Temperature sensitivity | Mild, intermittent | Noticeable and lingering | Intense and prolonged |
| Visibility | Not visible | Sometimes visible | Often visible or fractured |
| Risk to pulp | Low | Moderate | High |
| Treatment approach | Monitoring or minor restoration | Crown placement | Root canal or extraction |
Does a cracked tooth always hurt, or can it go unnoticed?
It’s a common assumption that if something is wrong with a tooth, it should hurt. But cracked teeth don’t follow that rule. In fact, some of the most clinically significant cracks produce little to no pain, at least initially. That’s where things become risky.
When a Cracked Tooth Causes No Pain
A crack that remains confined to the enamel may not trigger any symptoms at all. Enamel does not contain nerve endings, so damage at this level can go entirely unnoticed.
Patients often continue normal chewing habits without realizing there is a structural compromise. In some cases, cracks are only discovered during routine dental exams or imaging performed for unrelated reasons.
Clinical observations referenced by the American Association of Endodontists indicate that asymptomatic cracks are not uncommon, particularly in early stages.
The Role of Nerve Involvement
Pain typically begins when the crack extends into the dentin or reaches the pulp. The dentin contains microscopic tubules that connect to the nerve, making the tooth responsive to external stimuli.
But here’s the nuance, nerve involvement does not always produce constant pain. Instead, patients may experience:
- Occasional discomfort under pressure
- Sensitivity that appears and disappears
- Delayed pain after chewing
In some cases, the pulp may become necrotic (non-vital), eliminating pain entirely while infection develops silently.
Silent Damage and Long-Term Risk
The absence of pain does not mean the absence of damage. In fact, silent cracks can progress more dangerously because they remain untreated.
Over time, these cracks may:
- Deepen under repeated chewing forces
- Allow bacteria to infiltrate the pulp
- Lead to infection or abscess formation
Studies on cracked tooth syndrome emphasize that delayed diagnosis is a major factor in poor outcomes. What starts as a minor, painless crack can evolve into a condition requiring root canal therapy or extraction.
Why Some Patients Feel Nothing at All
Several factors influence whether a cracked tooth produces symptoms:
- The depth and direction of the crack
- The tooth’s location in the mouth
- Individual pain sensitivity
- Whether the pulp is still vital
This variability explains why two patients with similar cracks may have completely different experiences.
What are the main causes of cracked tooth toothaches?
A cracked tooth doesn’t always hurt, but when it does, there’s usually a clear mechanical or biological reason behind it. Toothaches related to cracks are typically triggered by movement within the tooth structure or irritation of the pulp.
Step 1: Mechanical Stress on the Tooth
Everything often begins with pressure. Chewing, biting, or clenching applies force to the tooth. If a crack is present, even a microscopic one, that force causes the tooth structure to flex.
This movement can irritate the inner tissues, especially when pressure is released. That’s why many patients feel pain after biting rather than during.
Step 2: Exposure of the Dentin Layer
As the crack progresses, it may expose the dentin. This layer is highly sensitive due to its connection to the nerve via dentinal tubules.
At this stage, patients may begin to notice:
- Sensitivity to cold or hot foods
- Discomfort when eating sweets
- Lingering pain after exposure to stimuli
Research published in the Journal of Endodontics highlights dentin exposure as a key factor in symptom development.
Step 3: Pulp Irritation and Inflammation
When the crack reaches deeper into the tooth, it can affect the pulp. This is where pain becomes more persistent and noticeable.
Inflammation of the pulp (pulpitis) can cause:
- Throbbing or aching pain
- Increased sensitivity to temperature
- Discomfort that may occur without chewing
If untreated, this inflammation can progress to infection.
Step 4: Bacterial Infiltration
Cracks create pathways for bacteria to enter the tooth. Once bacteria reach the pulp, infection can develop, leading to more severe symptoms.
At this stage, patients may experience:
- Constant pain
- Swelling in the surrounding tissues
- Sensitivity to pressure
The American Association of Endodontists notes that bacterial invasion is a critical turning point in the progression of cracked teeth.
Step 5: Structural Instability
As the crack deepens, the tooth becomes structurally compromised. Larger segments of the tooth may begin to move independently under pressure.
This instability amplifies pain and increases the risk of fracture.
Why are my teeth cracking all of a sudden?
Sudden tooth cracking often feels alarming, especially when there has been no obvious injury. But in many cases, the process has been developing quietly over time.
Aging and Natural Wear
Teeth are strong but not immune to wear. Over the years, enamel gradually becomes more brittle due to repeated stress and exposure to acids.
This makes teeth more susceptible to cracking, even during normal activities like chewing.
Bruxism (Teeth Grinding and Clenching)
Grinding exerts a significant force on teeth, often far greater than normal chewing. Over time, this repeated pressure can create microcracks that eventually become symptomatic.
Many patients are unaware they grind their teeth, especially if it occurs during sleep.
Large Fillings and Previous Dental Work
Teeth that have undergone extensive restorations are structurally weaker. Large fillings reduce the amount of natural tooth structure, making the remaining enamel more prone to cracking.
Clinical data suggest that heavily restored teeth are at higher risk of fracture under normal biting forces.
Dietary Habits and Sudden Stress
Certain eating habits increase the likelihood of cracks:
- Chewing ice or hard candies
- Biting down on hard foods unexpectedly
- Frequent temperature changes (hot coffee followed by cold water)
These actions can create sudden stress within the tooth structure.
Causes of Sudden Tooth Cracks
| Cause | Mechanism | Risk Level | Common Indicators |
|---|---|---|---|
| Aging enamel | Gradual weakening of tooth structure | Moderate | Increased sensitivity, minor cracks |
| Bruxism | Repetitive excessive force | High | Jaw soreness, worn teeth |
| Large fillings | Reduced structural support | High | Cracks around restorations |
| Hard foods | Sudden impact stress | Moderate to High | Immediate pain after biting |
| Temperature changes | Expansion and contraction stress | Low to Moderate | Sensitivity to hot/cold |
Looking at the Bigger Picture
What feels sudden is often the result of cumulative stress. Teeth rarely crack without a reason; the signs were likely there, just not obvious.
From a clinical standpoint, identifying the underlying cause is essential. Without addressing it, even treated teeth remain at risk of further damage.
How can you tell if a cracked molar has become infected?
There’s a turning point patients often remember not when the crack first appeared, but when something changed. The discomfort becomes harder to ignore, the symptoms more persistent, and the tooth starts to feel like a source of pressure rather than just sensitivity. That shift often signals infection.
Key Signs of Infection
Once bacteria enter through a crack and reach the pulp, infection can develop within the tooth and surrounding tissues. At this stage, symptoms tend to intensify and become more consistent.
Common warning signs include:
- Persistent or throbbing pain that does not subside
- Swelling in the gums or face near the affected tooth
- A bad taste in the mouth or foul odour
- Presence of pus or a small pimple-like bump on the gums (fistula)
- Increased sensitivity to pressure when biting
According to clinical guidance from the American Association of Endodontists, these symptoms are strongly associated with pulpal infection or abscess formation.
Swelling and Pressure: What They Indicate
Swelling is not just a surface-level issue; it often reflects deeper infection spreading beyond the tooth. Patients may notice:
- Tenderness in the jaw
- Difficulty opening the mouth fully
- A feeling of pressure around the tooth
This occurs when infection extends into the surrounding bone or soft tissue. At this point, prompt treatment becomes critical.
Taste and Drainage: A Subtle but Serious Sign
A persistent bad taste can be one of the earliest indicators of infection. This often results from pus draining from the infected site into the mouth.
While the drainage may temporarily reduce pressure and pain, it does not resolve the infection. In fact, it indicates that the body is attempting to manage a localized abscess.
Early Diagnostic Warning Signs Dentists Look For
Dentists rely on a combination of visible signs and patient-reported symptoms to identify infection early. These include:
- Localized swelling or redness of the gums
- Sensitivity to percussion (tapping on the tooth)
- Changes in tooth colour (possible pulp necrosis)
- Radiographic evidence of bone loss near the root
Early identification allows interventions, such as root canal therapy, to be undertaken before the infection spreads further.
How do dentists diagnose a cracked tooth accurately?
Diagnosing a cracked tooth is rarely straightforward. Unlike cavities or fractures that are clearly visible, cracks can be microscopic or hidden below the surface. That’s why dentists rely on a combination of methods rather than a single test.
Bite Tests and Symptom Reproduction
One of the most effective diagnostic tools is the bite test. Patients are asked to bite down on a small instrument designed to isolate pressure on specific parts of the tooth.
If a crack is present, this test often reproduces the characteristic pain, especially when pressure is released.
This method helps:
- Identify the specific tooth involved
- Determine which cusp is affected
- Confirm pressure-related pain patterns
Visual Aids: Dye and Transillumination
To enhance visibility, dentists may apply special dyes that seep into cracks, making them easier to detect. Another technique, transillumination, involves shining a bright light through the tooth.
Cracks disrupt the way light travels, revealing otherwise invisible structural defects.
These methods are particularly useful for detecting:
- Hairline cracks
- Craze lines
- Fractures not visible on X-rays
The Role and Limitations of X-rays
X-rays are essential for evaluating the overall health of the tooth and surrounding structures. However, they have limitations in detecting cracks.
Because cracks are often too thin or oriented in certain directions, they may not appear on standard radiographs.
Instead, X-rays are used to:
- Identify signs of infection or bone loss
- Assess previous dental work
- Rule out other conditions
Clinical Diagnostic Process in Practice
In a clinical setting, diagnosis is a layered process. Dentists combine multiple data points to reach a conclusion.
This typically involves:
- Reviewing patient history and symptom patterns
- Performing targeted bite and percussion tests
- Using visual enhancement tools
- Interpreting radiographic findings
Research in the Journal of Endodontics emphasizes that no single method is sufficient — accurate diagnosis depends on correlating clinical findings with patient-reported experiences.
What happens if you ignore a cracked tooth for too long?
It’s easy to delay action when symptoms are mild or inconsistent. But cracked teeth rarely remain stable. Over time, small structural defects tend to worsen, often leading to more complex and invasive treatments.
Progressive Structural Damage
A crack that starts in the enamel can gradually extend deeper with repeated chewing forces. Each bite places stress on the tooth, causing the crack to widen or lengthen.
Eventually, this may lead to:
- Splitting of the tooth structure
- Loss of structural integrity
- Increased mobility of tooth segments
At this stage, restorative options become more limited.
Increased Risk of Infection
As cracks deepen, they create pathways for bacteria to enter the pulp. Once infection sets in, the situation becomes significantly more serious.
Patients may experience:
- Persistent pain
- Swelling or abscess formation
- Systemic symptoms in severe cases
Clinical data consistently show that untreated cracks are a major risk factor for endodontic complications.
Need for More Invasive Treatment
Early-stage cracks can often be managed with conservative treatments such as crowns. However, delayed intervention may require:
- Root canal therapy to remove infected pulp
- Surgical procedures in advanced cases
- Tooth extraction if the damage is irreversible
Each step represents an escalation in complexity, cost, and recovery time.
Worsening Pain and Functional Impact
Pain associated with cracked teeth tends to intensify over time. What begins as occasional discomfort can evolve into constant, disruptive pain.
Patients may find it difficult to:
- Eat normally
- Sleep comfortably
- Focus on daily activities
From a broader perspective, untreated dental issues can significantly impact quality of life.
A Broader Clinical Perspective
Studies from endodontic research highlight that early diagnosis and intervention are key predictors of successful outcomes. Waiting does not stabilize a crack; it allows it to progress.
What’s the takeaway? A cracked tooth is not a static condition. Without treatment, it progresses toward greater damage and more complex care.
What treatment options are available for cracked teeth?
Treatment decisions for cracked teeth are rarely one-size-fits-all. The appropriate approach depends on several clinical factors, such as how deep the crack extends, whether the pulp is involved, and how much of the tooth structure remains intact. The goal is always the same: stabilize the tooth, eliminate pain, and prevent further damage.
Bonding for Minor Cracks
For superficial cracks confined to the enamel, dental bonding may be sufficient. This involves applying a tooth-coloured resin to seal the crack and restore the surface.
Bonding is typically recommended when:
- The crack is small and non-structural
- There is minimal or no pain
- The tooth remains stable under pressure
While bonding can improve aesthetics and reduce sensitivity, it does not provide the same level of structural reinforcement as other options.
Crowns for Structural Protection
When cracks extend into the dentin or compromise the tooth’s strength, a crown is often the preferred treatment. A crown covers the entire tooth, redistributing biting forces and preventing the crack from spreading.
Clinical guidelines widely support crowns as a primary treatment for cracked tooth syndrome, especially when:
- Pain occurs during chewing
- The crack is visible or confirmed through testing
- There is a risk of further fracture
Crowns are considered a long-term solution and significantly improve prognosis when placed early.
Root Canal Therapy for Pulp Involvement
If the crack has reached the pulp and caused inflammation or infection, root canal therapy becomes necessary. This procedure removes the infected tissue, disinfects the canal, and seals the tooth.
Indications include:
- Persistent or spontaneous pain
- Sensitivity that lingers after stimuli are removed
- Evidence of infection on imaging
Following a root canal, a crown is usually placed to restore strength and function.
Extraction in Severe Cases
In situations where the crack extends below the gum line or splits the tooth entirely, extraction may be unavoidable.
This is typically considered when:
- The tooth cannot be structurally restored
- Infection has severely compromised the surrounding tissues
- The crack involves the root
Replacement options such as implants or bridges are then discussed to restore function.
Treatment Options for Cracked Teeth
| Treatment | Indication | Advantages | Limitations |
|---|---|---|---|
| Bonding | Minor enamel cracks | Minimally invasive, quick | Limited durability, not structural |
| Crown | Moderate cracks, structural weakness | Strong protection, long-term solution | Requires tooth preparation |
| Root Canal + Crown | Pulp involvement or infection | Eliminates pain, preserves the tooth | More complex procedure |
| Extraction | Severe or non-restorable cracks | Removes the infection source | Requires a replacement option |
Decision Factors Dentists Consider
Dentists evaluate several variables before recommending treatment:
- Depth and orientation of the crack
- Presence of symptoms or infection
- Location of the tooth in the mouth
- Patient’s bite force and habits (e.g., grinding)
The earlier the intervention, the more conservative the treatment can be.
How can you prevent cracks and protect your teeth long term?
Prevention often comes down to reducing stress on the teeth and maintaining their structural integrity over time. While not all cracks can be avoided, many risk factors are manageable with consistent care.
Protecting Teeth from Mechanical Stress
One of the most effective preventive measures is using a custom mouthguard, particularly for patients who grind or clench their teeth.
Mouthguards help:
- Distribute biting forces evenly
- Reduce pressure on individual teeth
- Prevent microcracks from forming or worsening
Night guards are especially important for patients with bruxism, even if symptoms are not immediately noticeable.
Dietary Habits and Daily Choices
Every day habits play a significant role in tooth integrity. Avoiding excessive force is key.
Risk-reducing habits include:
- Avoiding chewing ice, hard candies, or non-food objects
- Being cautious with hard or brittle foods
- Limiting rapid temperature changes (e.g., hot drinks followed by cold water)
Small adjustments can significantly reduce cumulative stress on teeth.
Regular Dental Checkups and Early Detection
Routine dental visits allow for early identification of cracks before symptoms develop. Dentists can monitor subtle changes and recommend preventive measures.
Preventive care includes:
- Professional examinations with magnification
- Monitoring existing restorations
- Early placement of protective restorations if needed
Prevention Strategies and Their Impact
| Prevention Method | Purpose | Benefit Level | Notes |
|---|---|---|---|
| Mouthguard | Reduce grinding force | High | Essential for bruxism patients |
| Diet control | Minimize sudden stress | Moderate | Avoid hard foods |
| Regular checkups | Early detection | High | Enables conservative treatment |
| Restorative maintenance | Strengthen weakened teeth | High | Important for teeth with fillings |
| Temperature awareness | Reduce expansion stress | Low to Moderate | Avoid extremes |
A Long-Term Perspective
Prevention is not a single action; it’s a combination of habits and clinical care. Over time, these measures reduce the likelihood of cracks forming and progressing.
What should you remember about cracked tooth symptoms?
Cracked teeth rarely present in a straightforward way. Symptoms can be subtle, inconsistent, and easy to overlook, especially in the early stages. But as the condition progresses, the risks increase, pain intensifies, infection may develop, and treatment becomes more complex.
Key Points to Remember
- Pain when chewing or releasing pressure is a common early sign
- Sensitivity to temperature may indicate deeper involvement
- Cracks can exist without pain but still pose serious risks
- Early diagnosis allows for more conservative treatment
Cracked Tooth Overview
| Aspect | Key Insight |
|---|---|
| Symptoms | Variable, often intermittent |
| Causes | Mechanical stress, aging, and restorations |
| Risks | Infection, structural failure |
| Treatments | Bonding, crowns, root canals, and extraction |
| Prevention | Mouthguards, diet, and regular dental care |
Expert Recommendations
Dental professionals consistently emphasize early evaluation. When symptoms are unclear or intermittent, it is still advisable to seek an assessment rather than wait for symptoms to progress.
Experts from our company recommend monitoring even minor discomfort and scheduling an examination when symptoms appear inconsistent or unexplained.
Final Thought
A cracked tooth is not a condition that resolves on its own. It evolves — sometimes slowly, sometimes suddenly. Understanding the symptoms and acting early can make the difference between a simple restoration and complex treatment.
FAQ
What are the first signs of a cracked tooth?
Early signs often include pain when biting or releasing pressure, sensitivity to hot or cold foods, and discomfort that comes and goes. Symptoms may be mild at first and easy to overlook.
Can a cracked tooth heal on its own?
No, a cracked tooth cannot heal naturally. Without treatment, the crack may worsen over time and lead to infection or tooth loss.
Why does a cracked tooth hurt when I bite down?
Pain occurs because the crack allows parts of the tooth to move slightly under pressure, irritating the inner pulp and nerve endings.
Is it possible to have a cracked tooth with no pain?
Yes, some cracks — especially those limited to enamel — may not cause any symptoms. However, they can still worsen over time if left untreated.
When should I see a dentist for a cracked tooth?
You should see a dentist as soon as you notice symptoms like pain when chewing, sensitivity, or unexplained discomfort. Early diagnosis helps prevent more serious complications.